JOIN #PROJECTPLAY
Sign up for our monthly newsletter
Project Play is anchored in the notion that all children and adolescents, regardless of zip code or ability, should have access to high-quality sport activity that allows them to develop as human beings. “Sports” refers to all forms of health-enhancing physical activity which, through organized or casual play, aims to express or improve physical fitness and mental well-being.
A mountain of evidence now documents the physical, mental, social, emotional, cognitive and academic benefits that flow to youth whose bodies are in motion. We also know communities thrive when they promote policies and develop infrastructure that encourage sport and recreation activity.
EXPLORE our report for current trends in youth sports
In this section, learn more about the benefits of sport and physical activity for youth. Project Play shares the latest participation rates and facts highlighting the challenges in getting and keeping youth playing, as well as the consequences of society failing to do so. Please click on the above tabs to explore each of these topics. Read our annual National State of Play report for the latest research and trends related to youth sports and physical activity.
Why Sport Matters Now …
The pandemic, social unrest, and rapid advance of technology have shifted the value proposition for why all children should have an opportunity to play, and develop as people, through sports. We gathered the latest research to help you make the case with stakeholders and unlock new funding and policy opportunities.
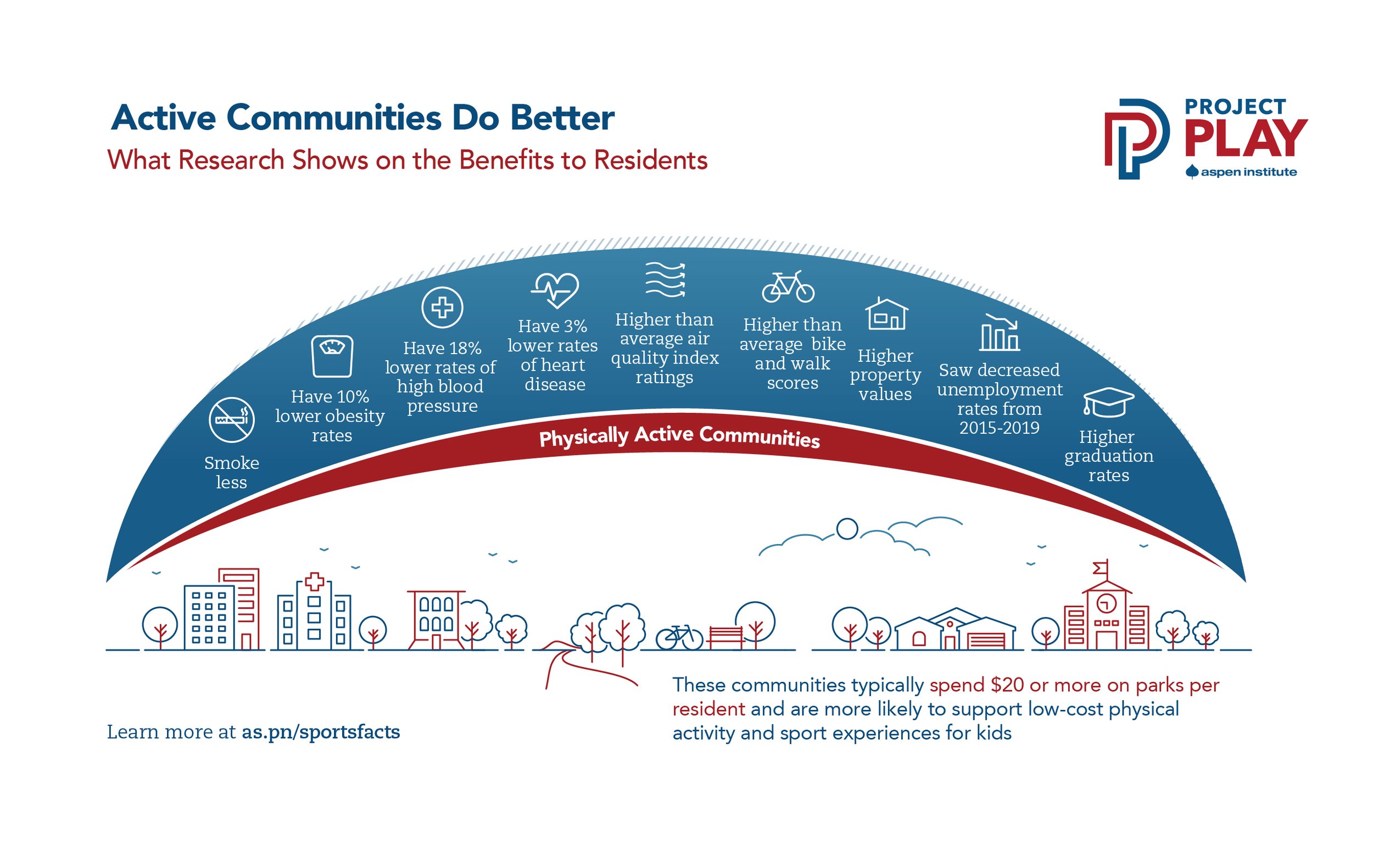
We also know that communities thrive when they promote policies and develop infrastructure that encourage sport and recreation. The below infographic by Project Play reflects some of benefits that flow to physically active communities.
For our purposes here, we define a “physically active community” as one that actively supports the health, social, and economic benefits of physical activity, sport, and recreation by promoting policies and infrastructure that encourage healthy behavior.
+ Graphics Methodology
We examined the top 10 cities (overall ranked) in the 2019 ACSM American Fitness Index to understand the values, capital and financial investments, and environments of a community that invests in sport and recreation. The cities with the highest scores are considered to have a strong community fitness, a concept comparable to individuals having strong personal fitness.
+ Graphics Sources
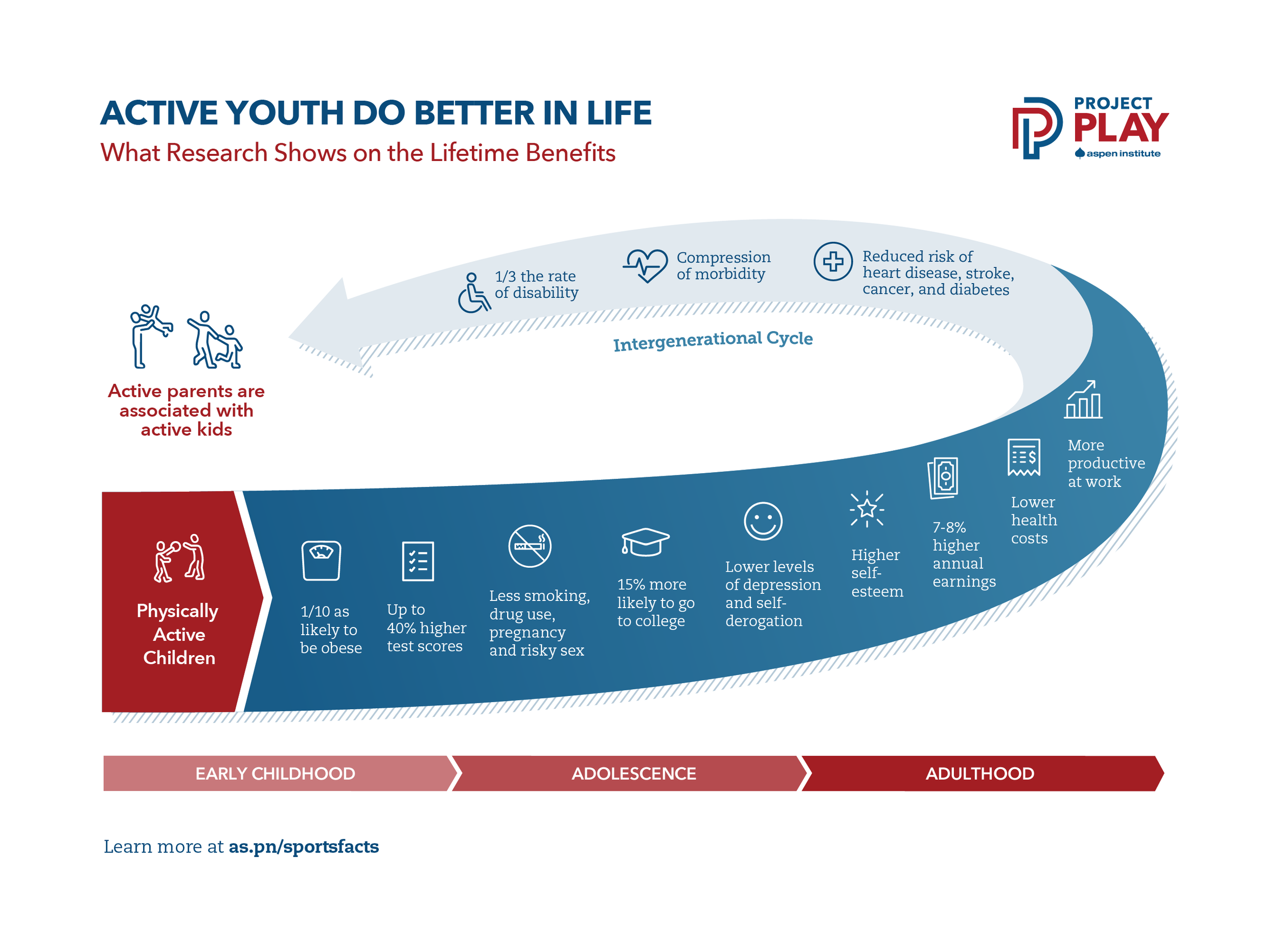
Active Kids Do Better In Life
Ratey, J. J., and Hagerman, E., Spark: The Revolutionary New Science of Exercise and the Brain, Little, Brown & Company, 2014.
Moore, L. et al., “Does early physical activity predict body fat change throughout childhood?,” Preventative Medicine, 37:10-17, 2003.
Grissom, J., “Physical Fitness and Academic Achievement,” Journal of Exercise Physiology, 8(1), 11-25, 2005.
Staurowsky, E.J., “Her Life Depends On It: Sport, Physical Activity, and the Health and Well-Being of American Girls and Women,” East Meadow, NY: Women’s Sports Foundation, 2009.
Jones-Palm, D.H. and Palm, J., “Physical Activity and Its Impact on Health Behavior among Youth,” 2005.
Lieras, C., “Do skills and behaviors in high school matter? The contribution of noncognitive factors in explaining differences in educational attainment and earnings,” Social Science Research, 27:888-902, 2008.
Stevenson, B., “Beyond the Classroom: Using Title IX to Measure the Return to High School Sports,” Review of Economics and Statistics, 92:284-301, 2010.
Cawley, J. and Meyerhoefer, C., “The medical care costs of obesity: An instrumental variables approach,” Journal of Health Economics, 31(1), 219-230, January 2012.
Proper, K.I. et al., “Dose-response relation between physical activity and sick leave,” British Journal of Sports Medicine, 40(2), 173-178, 2006; 2008 Physical Activity Guidelines for Americans, United States Department of Health and Human Services, 2008.
Olshansky, S.J. et al., “A Potential Decline in Life Expectancy in the United States in the 21st Century,” New England Journal of Medicine, 352(1):1138-1145, March 17, 2005.
Fires, J., “Physical activity, the compression of morbidity, and the health of the elderly,” Journal of the Royal Society of Medicine, 89, 64-68, 1996.
Moore, L.L. et al., “Influence of Parents’ Physical Activity Levels on Activity Levels of Young Children,” Journal of Pediatrics, 118(2):215-219, 1991.
Active Communities Do Better
American College of Sports Medicine. (2019, August 17). ACSM American Fitness Index.
Centers for Disease Control & Prevention. (2016, June 3). FastStats. National Center for Health Statistics: Obesity & Overweight.
Centers for Disease Control & Prevention. (2020, February 25). Facts About Hypertension | cdc.gov. High Blood Pressure: Facts About Hypertension.
Centers for Disease Control & Prevention. (2020b, June 22). Heart Disease Facts | cdc.gov. Heart Disease Facts.
National Recreation and Park Association. (2017). The Economic Impact of Local Parks | Research | National Recreation and Park Association. The Economic Impact of Parks: An Examination of the Economic Impacts of Operations and Capital Spending by Local Park and Recreation Agencies on the U.S. Economy.
U.S. Bureau of Labor Statistics. (2019, September 20). Unemployment Rates for Metropolitan Areas. Local Area Unemployment Statistics.
Open Data Network. (2018). High School Graduation Rate Data for Arlington, VA - Graduation Rates on the Open Data Network. High School Graduation Rates.
NPR, Robert Wood Johnson Foundation, & Harvard T.H. Chan School of Public Health. (2017, July 11). Sports and Health in America. Sports and Health in America.